Loco-regional Hyperthermia
Local hyperthermia (more accurately, modulated electro-hyperthermia or oncothermia, which is utilized in the ImunoMedica clinic) is currently regarded as the "fourth weapon in the fight against cancer" (German Cancer Aid).
It is one of the non-invasive anti-cancer therapies that works by targeting and destroying tumor cells while also boosting the immune system. The cancer tissue is heated to the point of necrosis or apoptosis throughout the treatment.
Another advantage of local hyperthermia is that it increases the responsiveness of cancerous tissue to standard cancer therapies, making it one of the most potent integrative anti-cancer therapies recognized and endorsed by the scientific community.
Local hyperthermia uses a weak point of the cancerous tumor, namely its inability to cope with high temperatures. Healthy tissue around the tumor regulates temperature by increasing blood flow and dilating blood vessels, while tumor tissue, on the contrary, experiences a decrease in blood circulation.
Therefore, for the tumor, the increase in temperature works as a trap, because it leads to the development of an acidic and harmful cellular environment, the inability to assimilate nutrients and self-intoxication. Thus, as part of exposure to local hyperthermia, overheating (temperatures between 41ºC and 43ºC) leads to a considerable disruption of tumor cell metabolism, which causes their death.
Procedure
In this form of therapy, ultrasounds or low frequency electrical currents are directed, in a controlled and targeted manner, by means of special devices, towards the organ or tissue affected by the tumor. The energy thus produced is absorbed by the extracellular environment where the tumor cells are located, consequently increasing their temperature and producing the intended effects.
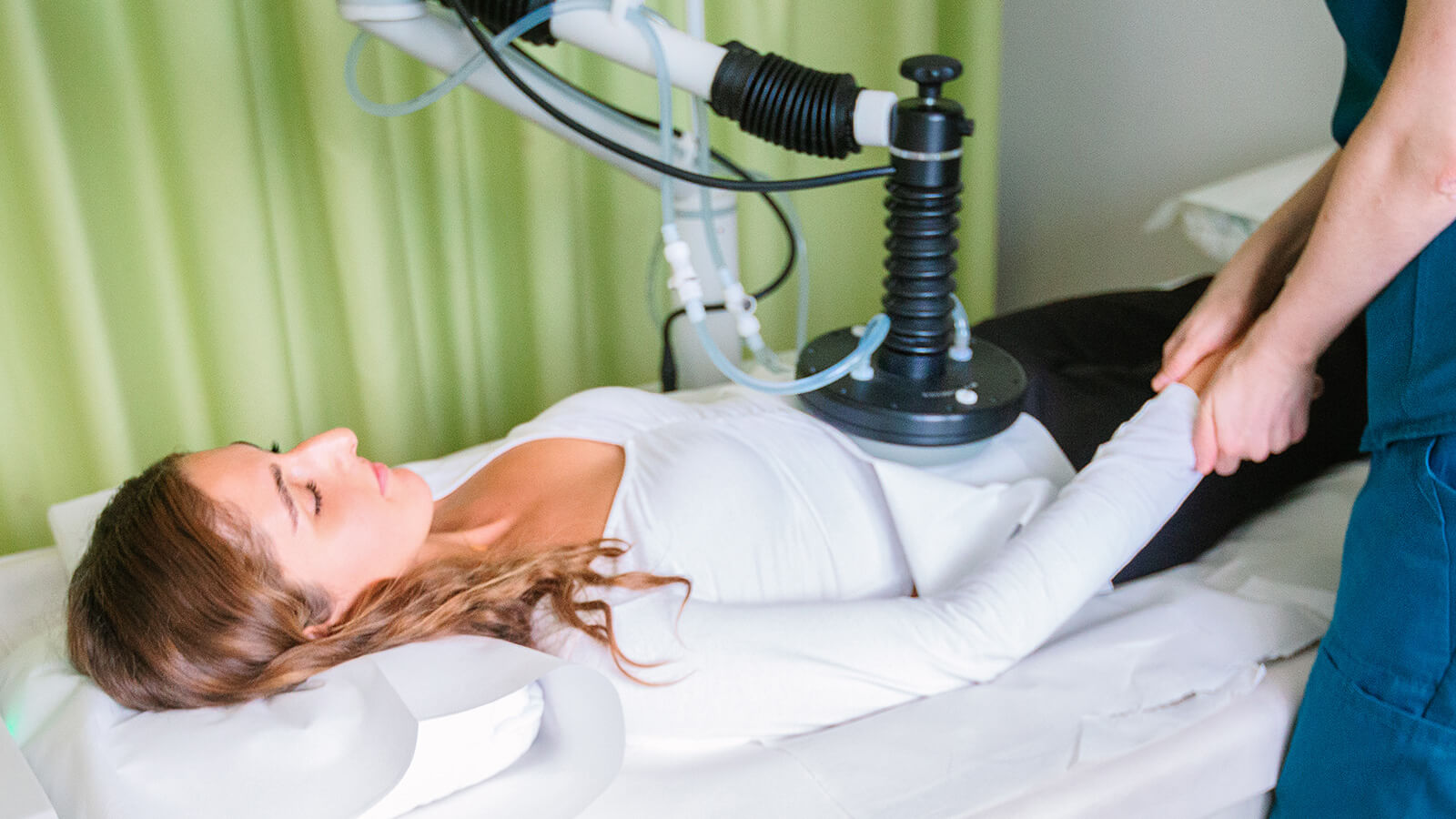
The devices that are used transmit the dose of energy in a controlled manner, causing the tissue to heat up to 42.5ºC.
Biophysics and cell biology tests have shown that, in tumor areas where cell activity is more intense, a higher ionic concentration is recorded. Therefore, the conductivity and permittivity of the extracellular matrix of malignant tissue becomes higher than in the healthy tissue. This difference facilitates the almost exclusive damage of the malignant cells in a tumor that also contains healthy cells. This natural selection is further accentuated by the individual behavior of the tumor cells, while also stimulating the immune response of the body.
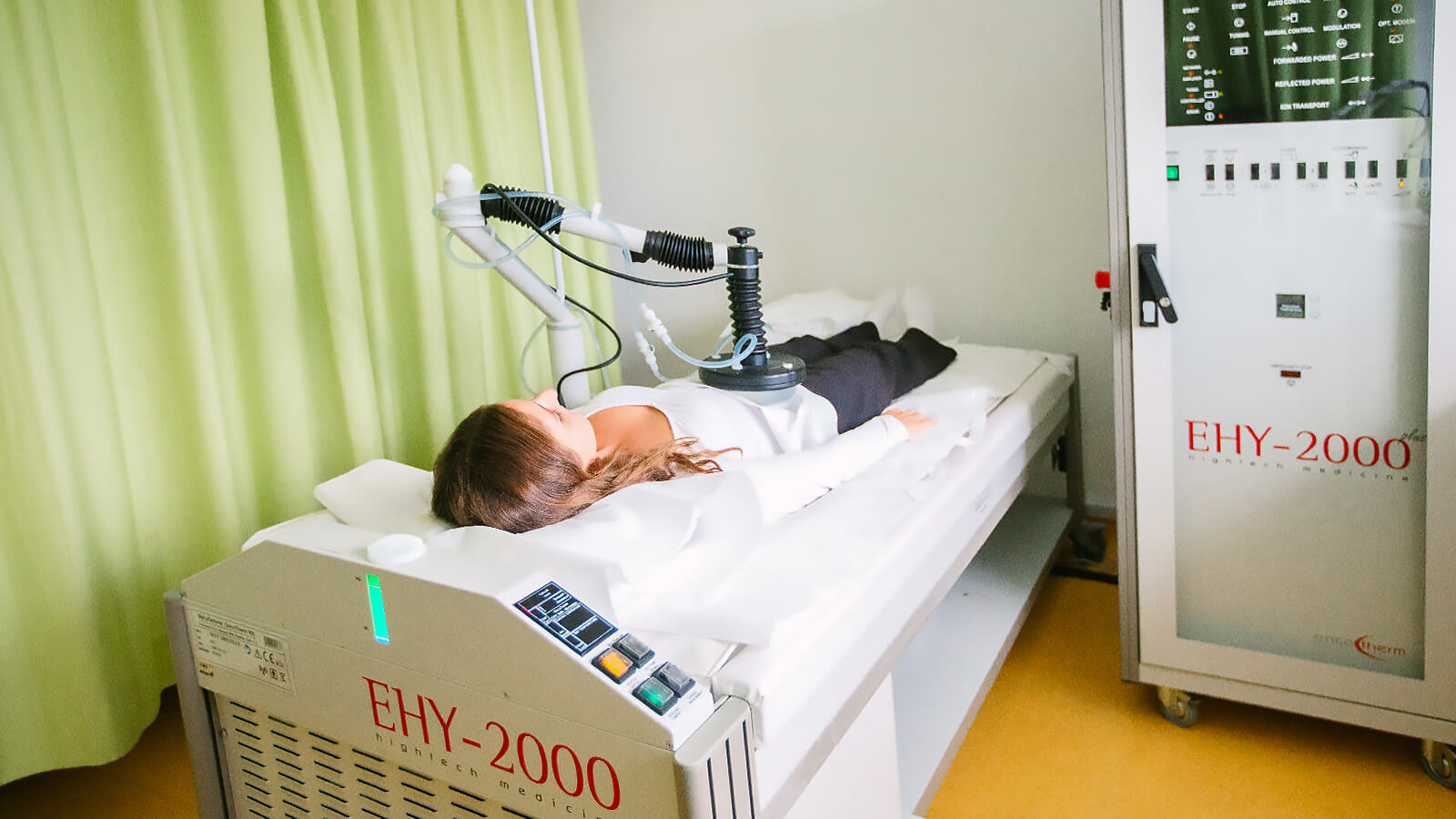
Local hyperthermia at the ImunoMedica clinic involves placing the patient on a special bed, between two different-sized condenser plates, between which an electric field is created at a frequency of 13.5 MHz.
Cancerous tissue and healthy tissue have different dielectric constants. Thus, the dielectric constant in cancerous tissue varies between 8 and 15 MHz, while the dielectric constant in healthy tissue varies between 80 and 100 MHz. The resonance vibration creates intense molecular friction and thus generates heat and increases the temperature of the tumor tissue. Therefore, the capacitive field of locally modulated electro-hyperthermia heats the tumor tissue, while only a moderate increase in temperature is observed in the surrounding healthy tissue. During the local hyperthermia session at the ImunoMedica clinic, which lasts approximately 60 minutes, the patient is under the continuous observation of the medical staff.
The frequency and duration of hyperthermia application depends entirely on the specific condition of the patient. Generally, therapy is extremely well tolerated. Usually, there are no side effects, even when used concomitantly with other therapies.
The heat is applied locally, directly to the affected tissue or organ. During the session, which lasts for approximately 60 minutes, the patient is placed on a special bed, under the continuous observation of the medical staff.
Recommendations
Clinical trials (phases II and III) have proven that loco-regional hyperthermia is recommended for solid tumors, both primary and metastatic. The therapy is able to increase the patient's survival rate and quality of life. It may also be applied for palliative purposes, when conventional therapies are no longer indicated or efficient.
Oncothermia is used in a large number of cancers, such as:
- breast cancer
- prostate cancer
- cancers with abdominal localization (stomach, intestine, liver, pancreas)
- lung cancer
- lymphatic cancer
- various other metastases.
Clinical experience has shown that local hyperthermia, especially when performed before or after tumor tissue removal surgery, improves patient recovery parameters and decreases the chances of subsequent metastasis occurrence.
Benefits
Chemosensitization
Local therapy, applied in addition to conventional chemotherapy, sensitizes the tumors to this treatment, by affecting the integrity of the tumor cell membrane and increasing the permeability and structural dysfunction, thus increasing the rate of absorption of the administered chemicals. The results of the clinical trials, phases II/III, proved that local hyperthermia, associated with chemotherapy, is a more precise way of targeted administering of antitumor drugs in the tumor.
Radiosensitization
Local hyperthermia sensitizes the tumor to radiotherapy when it is administered complementarily (there is an increase in oxygen supply to the cells). Regional hyperthermia carried out during radiotherapy treatments improves patients' response to treatment and their chances of survival. Hyperthermia increases oxygenation and thus reduces hypoxia, amplifying the cytotoxic effect of radiation. It also inhibits the processes of recovery of tumor cells affected by radiation.
Improves the immune response
Local hyperthermia activates antigen expression as a result of impaired tumor cell membrane. Most notably, the release of heat shock proteins (HSPs) that support the emergence of a tumor destruction immune response. The release, by the affected tumor cells, of the B1 proteins (HMGB1), ATP and HSP stimulates the body's immune response and thus contributes to the antitumor effect. Local hyperthermia also stimulates the restoration of inter-cellular and intermolecular connections necessary to trigger apoptosis (programmed cell death) and to stop the migration processes of tumor cells in the body.
Gene damage
Studies have shown that local hyperthermia activates the p53 suppressor tumor gene, which plays a role in lowering the rate of division and in facilitating apoptosis.
Side effects and contraindications
The therapy has minimal risks during administration, and side effects are limited and rare. The application of high temperature to the tumor has minimal effects on the neighboring healthy tissues.
From among side effects, the most common is the slight reddening of the area where the treatment was applied, but the effect disappears by itself due to the function of the highly branched and efficient blood system from healthy tissues. This does not happen in the tumor, as it is irrigated by a deficient capillary system.
The therapy is effective in all forms of cancer, but it is not recommended to be applied in areas where there is a pacemaker or metal stents placed in parallel to the electrode, as well as metal prostheses. Therapy may be applied from the distance of approximately 10-20 cm from these areas.
The therapeutic solutions we provide
Comprise a wide range of conventional, adjuvant and supportive therapies, which integrate medical concepts that have been built on a sturdy scientific basis and on the clinical experience of numerous cancer specialists worldwide.
ImunoMedica patients have access to the latest diagnostic tools, technologies and innovations as well as to the latest and best treatments available, as soon as these are proven to be safe and effective.
How can you become a patient of our clinic?
Throughout the whole process, from your initial contact, through treatment and after you leave our clinic, our patient coordinators will guide you through the steps and support you with all their expertise, attention and kindness.
*
We are here to help you
Our patient coordinator will contact you soon
Phone: +40.771.518.946, e-mail: office@imuno-medica.ro